Drug Delivery System (DDS) aims to achieve an effective and safe carrying of pharmaceutical compounds by controlling the dosage, route, and timing of administration in the body’s internal environment. We study transportation of drugs via transdermal route (transdermal DDS, TDDS) to the systemic circulation, or to the local dendritic cells. TDDS improves patient’s wellness and convenience, which has been an issue with the traditional drug administration method of injection.
Research
What is Drug Delivery System?
Controlling the skin permeation of the pharmaceutical molecules
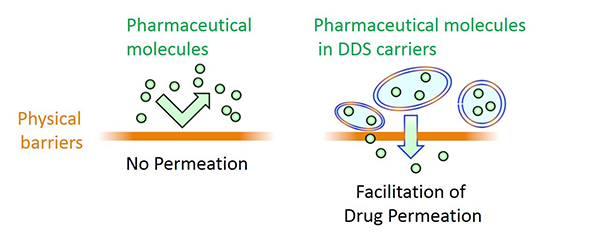
The human skin includes a keratinous layer, which has a barrier-function to protect the body from invasion of germs, viruses, and foreign molecules. Numbers of approaches have been developed to overcome the skin barrier, including physical and chemical methods. For example ultrasound, electroporation, and microneedle arrays, are classified as physical transdermal permeation methods. On the other hand, techniques that use chemically modified nano-sized particles, vesicles, or molecules are classified as chemical transdermal permeation methods. In our laboratory, we have developed a nano-sized lyophilized powder of hydrophilic pharmaceutical molecules coated with hydrophobic surfactants in oil-vehicle to facilitate drug permeation into the skin.
|
Solid-in-oil (S/O) nanodispersion system
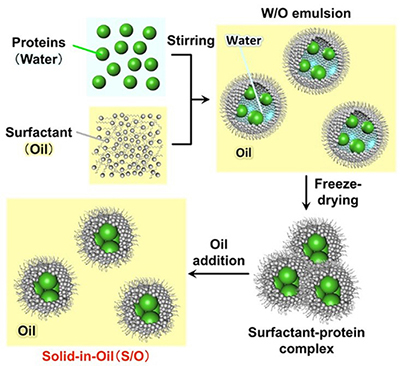
Solid-in-oil nanodispersion system is composed of a nano-sized particle containing hydrophilic molecules covered with hydrophobic surfactants, dispersed in an oil-vehicle. Using the S/O nanodispersion system, we achieved an enhanced permeation of the hydrophilic molecules into the skin. Further improvements of permeation efficiency, and application to wide variety of areas including transcutaneous immunization system are now being examined.
|
| Preparation of the solid-in-oil nanodispersions. |
Transdermal delivery of pharmaceutical compounds and proteins
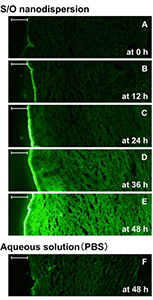
Insulin (Mw: 6000) is a large hydrophilic protein, which usually does not overcome the skin barrier. However, we have succeeded to permeate this protein into the skin by using our novel S/O nanodispersion system. The follow figure shows the permeation of the fluorescence dye-labeled insulin deep into the pig skin varying over time. The protein permeated in the skin retained its activity, indicating that the protein can serve as a drug after transdermal administration. Transdermal administration of other pharmaceutical compounds, including diclofenac, are also being studied using the S/O nanodispersion system.
|
| Permeation of the fluorescence dye-labeled insulin into the pig skin was observed by fluorescence microscopy. (bar=200 μm) M. Goto et al., J. Control. Release, 131, 14 (2008). |
Transdermal delivery of vaccines
Vaccines are administered to prevent the infection of germs or viruses, or to improve the immune system and reduce symptoms of infectious diseases. Moreover, vaccination is considered to be applicable for the therapy of allergic diseases or cancers. Large sizes of molecules, such as viruses, proteins, and peptides are used as vaccines, thus, transcutaneous delivery of the vaccine molecules have been limited. Nevertheless, in our laboratory, we could induce antigen-specific immune response by the transcutaneous administration of the antigen model protein, ovalbumin, and by the use of the skin’s immune system.

|
|
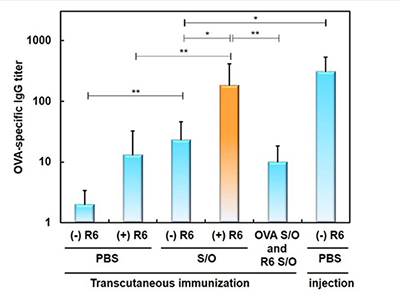
| An enhanced permeation of ovalbumin was achieved by the optimization of the S/O nanodispersion system. M. Goto et al., Med. Chem. Commun., 5, 20 (2013) |
Induction of the anti-ovalbumin (OVA) specific antibody increased by the co-encapsulation of the polyarginine (R6) in the S/O nanoparticles. M. Goto et al., Int. J. Pharm.,458, 334 (2013) |
Transcutaneous delivery of cosmetic compounds
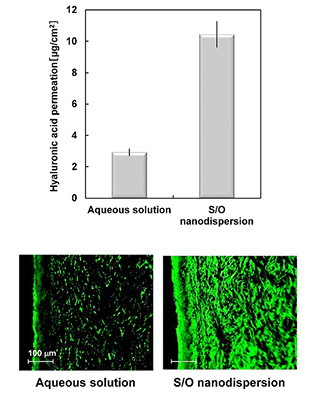
Using the S/O nanodispersion system, we have also achieved the transcutaneous delivery of cosmetic compounds, vitamin C, and hyaluronic acid. This progress resulted in the commercialization of the cosmetic products (Product name: VIVCO). We are now addressing the transcutaneous delivery of a variety of cosmetic compounds.
|
| Here we could verify the amount of hyaluronic acid permeated in the pig skin (up figure), and through microscopic observation of the pig skin treated with fluorescence dye-labeled hyaluronic acid (bottom figure). 後藤雅宏ほか,膜(Membraane),36(2),57 (2011) 後藤雅宏,ファインケミカル,39,49 (2010) |

